  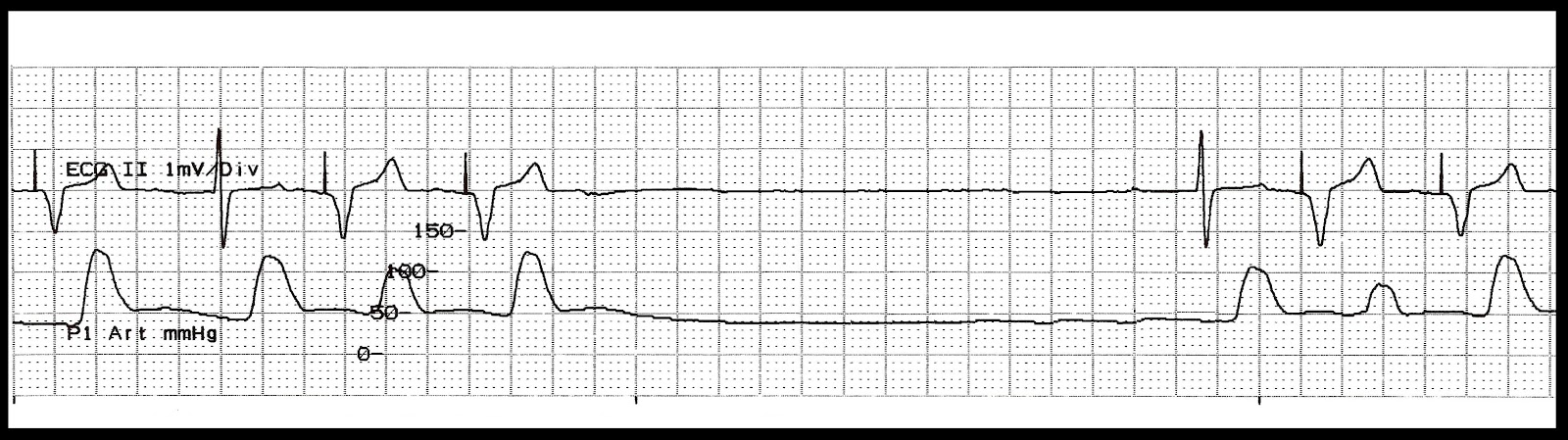
US National Guidelines Clearinghouse on The EKG in a patient with a pacemaker Trial results on The EKG in a patient with a pacemakerĬlinical Trials on The EKG in a patient with a pacemaker at Google Ongoing Trials on The EKG in a patient with a pacemaker at Clinical TRIP on The EKG in a patient with a pacemaker Videos on The EKG in a patient with a pacemakerĬochrane Collaboration on The EKG in a patient with a pacemakerīandolier on The EKG in a patient with a pacemaker Podcasts & MP3s on The EKG in a patient with a pacemaker Photos of The EKG in a patient with a pacemaker Images of The EKG in a patient with a pacemaker Powerpoint slides on The EKG in a patient with a pacemaker Review articles on The EKG in a patient with a pacemakerĪrticles on The EKG in a patient with a pacemaker in N Eng J Med, Lancet, BMJ Most cited articles on The EKG in a patient with a pacemaker Most recent articles on The EKG in a patient with a pacemaker Multiple causes including oversensing, wire fracture, lead displacement, or interference.įailure to capture occurs when paced stimulus does not result in myocardial depolarisation.WikiDoc Resources for The EKG in a patient with a pacemaker Results in decreased or absent pacemaker function. Output failure occurs when a paced stimulus is not generated in a situation where expected. Reduced pacemaker output / output failure may be seen on ECG monitoring if the patient stimulates their rectus or pectoral muscles (due to oversensing of muscle activity). These inappropriate signals may be large P or T waves, skeletal muscle activity or lead contact problems.Ībnormal signals may not be evident on ECG. Oversensing occurs when electrical signal are inappropriately recognised as native cardiac activity and pacing is inhibited. Undersensing occurs when the pacemaker fails to sense native cardiac activity.Ĭauses include increased stimulation threshold at electrode site (exit block), poor lead contact, new bundle branch block or programming problems.ĮCG findings may be minimal, although presence of pacing spikes within QRS complexes is suggestive of undersensing. Pacemaker malfunction can occur for a wide variety of reasons, ranging from equipment failure to changes in underlying native rhythm.ĭiagnosis of pacemaker malfunction is challenging and often associated with non-specific clinical symptoms while ECG changes can be subtle or absent. Underlying rhythm left on its own, with a long pause followed by a ventricular escape beat. The ekg strip below shows the first two spikes pacing, then the pacemaker fails to pace. Its absence will result in the underlying rhythm running (if any). It may be the pacemaker battery, the leads or it could be an over sensing problem. In general, you will have no pacing spikes where they need to be. It could be an intermittent problem or failure altogether. There is no particular rhythm to define this. 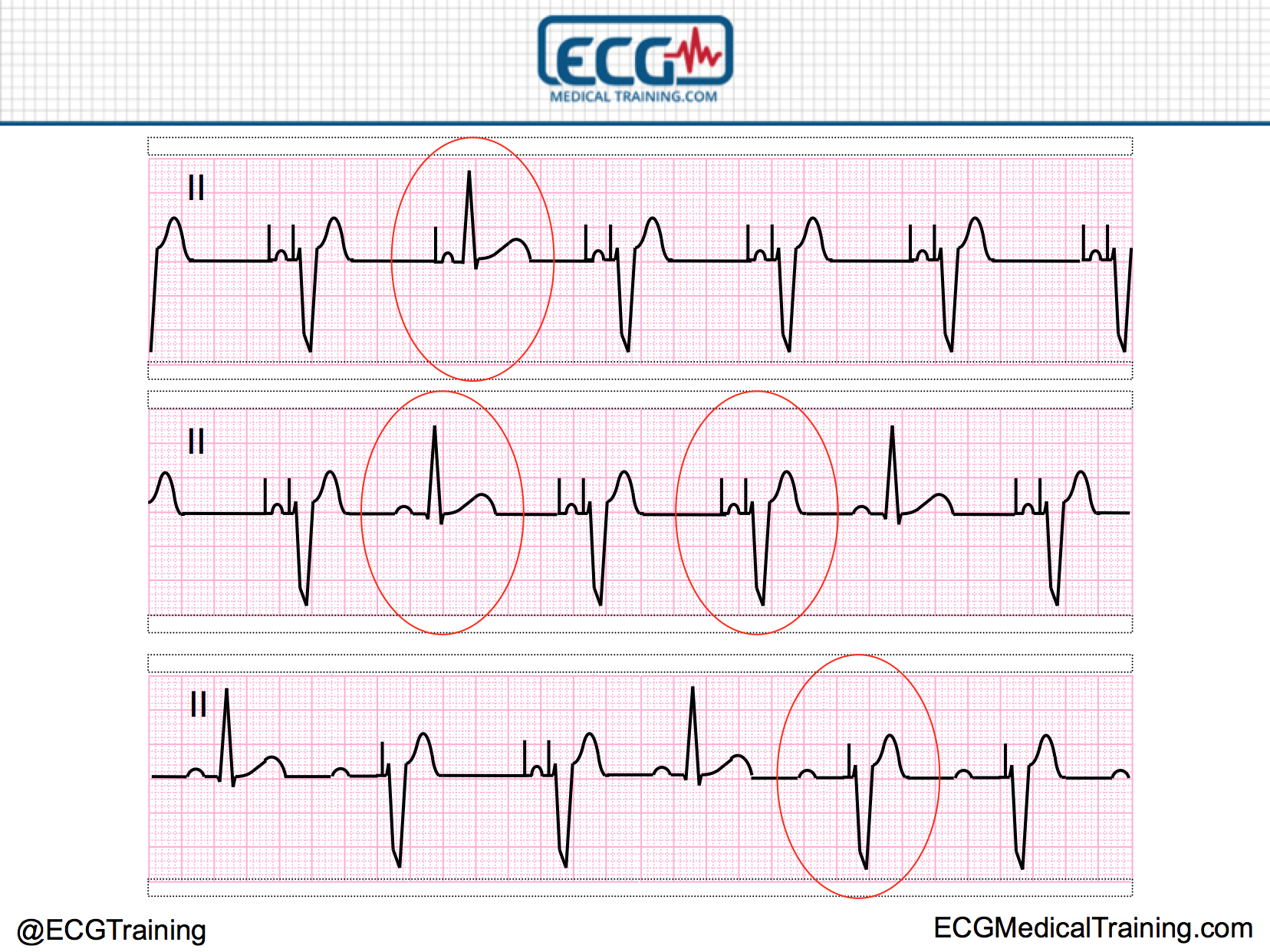
Somehow, the electrodes have no current flowing through them. Spikes are sensing correctly and pace the ventricles.įailure to output (failure to pace) simply means there is no output signal being generated from the pacemaker. (undersensing) shows the first two spikes fire out of place. Sensing issues are identified when there are pacemaker spikes showing up where they do not belong. Which occurs when a foreign signal (non-cardiac) such as a muscle twitch, are mistaken for real cardiac activity. Sensing problems include “undersensing” where the pacemaker fails to sense the native cardiac rhythm. In most cases, sensing problems are less threatening and can be corrected by performing a pacemaker interrogation. The example below shows the first two ventricular paced beats capture, then the next This is identified by having pacing spikes present with no resulting QRS, (capture). Failure to capture is when the pacemaker signal fires but there is no response. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
